Spina bifida occulta (also known as closed spina bifida) refers to malformations where the neural tissues are coved with skin. This class of spina bifida is quite common (seen in 20 to 30 percent of Americans) and is frequently of little or no clinical significance and it is rare when patients have an associated neurological defecit. A minority of patients with spina bifida occulta will have a developmental anomaly of the spinal cord such as: splitting of the spinal cord (diastomatomyelia), tethering of the spinal cord (abnormally low position of the spinal cord), and tumors involving the spinal cord such as a dermoid or a lipoma, or even a dermal sinus tract.
Spina bifida aperta (also known as open spina bifida) refers to malformations where the neural tissues are not covered with skin. There are two basic types of spina bifida aperta: meningocele and myelomeningocele. In a meningocele, only the membranes covering the neural elements herniate through the defect in the spinal column. In a myelomeningocele the neural elements and their covering membranes herniate through the defect in the spinal column. Only one third of patients with meningoceles may have neurological defecits since the neural elements do not herniate through the defect in the spinal column. In contrast, almost all patients with myelomeningocles are afflicted with a spectrum of sensory loss and leg weakness as well as bowel and bladder incontinence. The severity of the neurological deficit depends on the location of the spinal defect. The higher the defect is on the spinal column the greater the neurological injury since a wider array of nerves are affected. Patients with spina bifida aperta may also suffer from associated hydrocephalus and chiari malformations.
What Causes Spina Bifida?
Both environment and genetics are felt to play a part in spina bifida. Overall, only one in one thousand live births is afflicted with spina bifida aperta. However the risk of spina bifida aperta increases by a factor of 10 or 20 if one or more siblings are afflicted with spina bifida. Also diet and nutrition may influence the development of spina bifida. Folate deficiency, for example, has been cited as a cause of spina bifida.
How Is Spina Bifida Diagnosed?
The diagnosis of spina bifida aperta is frequently made during routine prenatal screening. High resolution ultrasound together with elevated serum levels of maternal alpha fetal protein frequently detect children afflicted with spina bifida prior to birth.
Spina bifida occulta is frequently discovered after birth. Usually it is an incidental finding of little clinical significance, however some patients may have an associated abnormality of the spinal cord and nerves such as: splitting of the spinal cord (diastomatomyelia), tethering of the spinal cord (abnormally low position of the spinal cord), a tumor involving the spinal cord such as a dermoid or a lipoma, or even a dermal sinus tract. These abnormalities frequently come to clinical attention when patients begin to experience some of the following symptoms: back pain, bowel and bladder incontinence, loss of sensation and weakness in the lower extremities. MRI of the spine is critical to both diagnosis and surgical planning in these patients.
How Is Spina Bifida Treated?
Spina bifida aperta usually requires timely surgical repair to avoid infections. The exposed neural tissue and membranes become colonized with bacteria if not promptly repaired potentially resulting in meningitis. The surgery usually involves mobilization and anatomic reconstruction of the exposed neural tissue followed by coverage with adjacent skin. Some patients with hydrocephalus or chiari malformations may require additional operations to treat these associated disorders.
Many patients with spina bifida occulta do not require treatment. Patients with an associated symptomatic abnormality of the spinal cord (such as a dermoid, lipoma, tethered cord, or split spinal cord) require surgical repair to prevent further neurological decline.
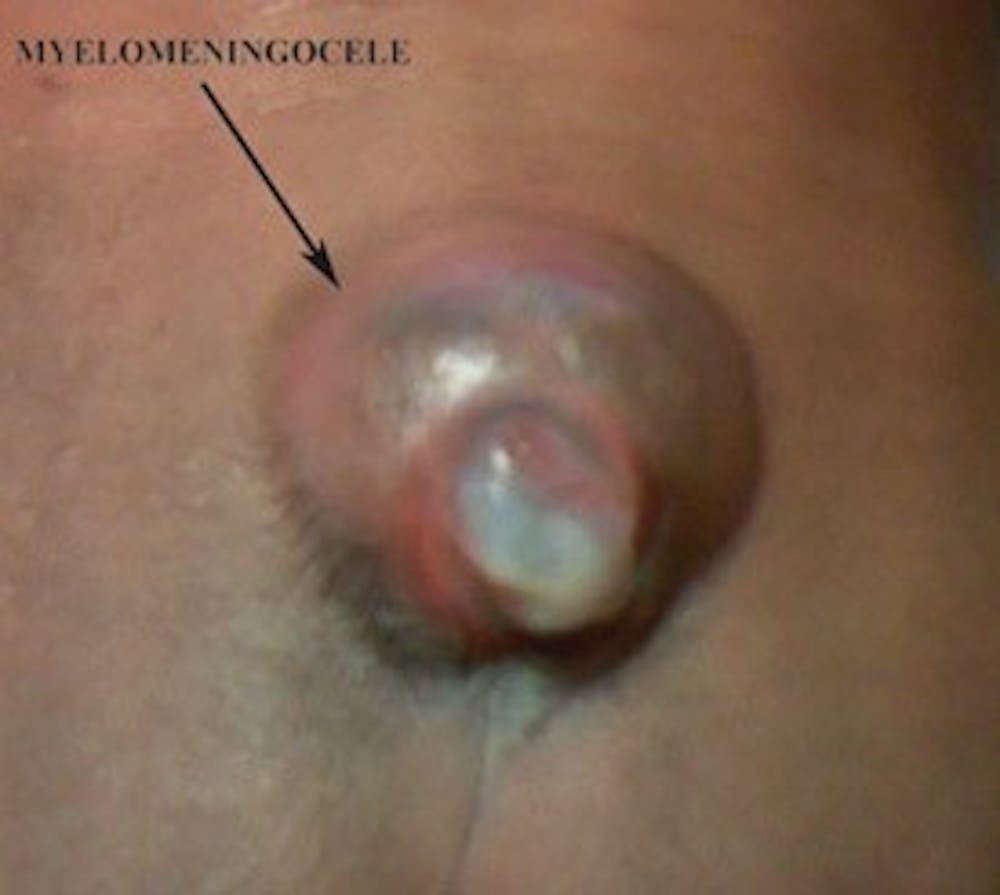
Pre-operative photo of a myelomeningocele in the lumbosacral region.