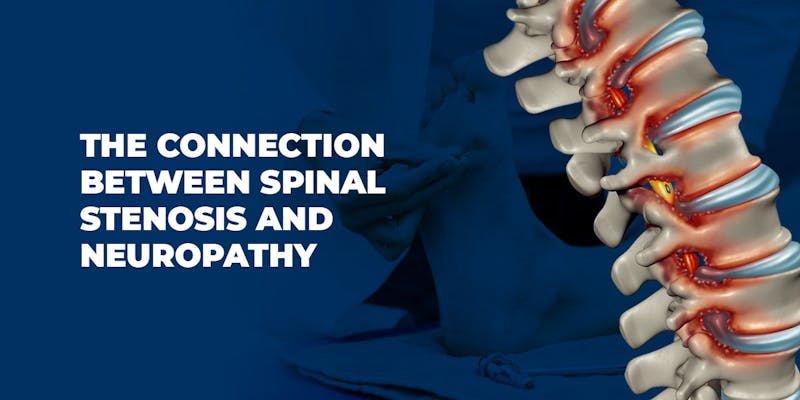
Spinal stenosis occurs when the spaces between the spine begin to narrow, limiting the ability for nerves to move through the spine. While it usually occurs in older individuals, younger people with spinal conditions or injuries can also develop spinal stenosis.
Meanwhile, neuropathy results from damage to the nerves outside of the brain or spinal cord. Its symptoms can vary depending on the person and underlying cause, but they may include:
- A prickling, tingling or burning sensation
- Temporary or permanent numbness
- Pain
- Heightened sensitivity to touch
- Muscle weakness
- Paralysis
- Organ or gland dysfunctions
- Problems with urination or sexual function
Neuropathy stems from various conditions including nutritional or vitamin imbalances, toxin exposure, medication effects, alcoholism and diabetes. But is there a link between spinal stenosis and neuropathy? Read on to discover how and why these conditions often go hand in hand.
What Causes Spinal Stenosis?
While some people are born with small spinal canals, spinal stenosis usually stems from medical conditions or injuries that constrict the openings between the spine. Here are some common causes of spinal stenosis:
- Osteoarthritis: Osteoarthritis is a common form of arthritis that wears down joint tissues over time. It frequently causes spinal stenosis.
- Herniated disc: Your discs absorb shock between the spinal bones. A herniated disc occurs when the spine vertebrae’s delicate inner casings shift out of place, damaging and drying out the disc. As a result, it can crack and discharge soft inner material, compressing the spinal cord and nerves.
- Spinal fractures: Trauma from a fall, car accident, sports injury or another incident can dislocate or fracture the spinal bones. The swelling of surrounding tissue after back surgery can put pressure on the spinal cord or nerves.
- Spinal tumors: Though a rare occurrence, tumors can develop within or between the spinal cord and lead to spinal stenosis. These growths can reduce the space between the cord and vertebrae, causing intense nerve pressure.
- Scoliosis: Scoliosis is a medical condition causing a sideways curvature of the spine. It can cause disc and joint degeneration, potentially resulting in spinal stenosis.
- Thick ligaments: Ligaments help hold the spinal bones together. They can sometimes grow stiff and thick over time, bulging into the spinal canal as a result.
- Bone spurs: Medical conditions like Paget’s disease of bone and arthritis can cause bone spurs — smooth, hard bumps that develop on the ends of bones. Bone spurs can move into the spinal canal.
Symptoms of Spinal Stenosis
Some people don’t encounter symptoms of spinal stenosis, at least not at first. The narrowing of the spinal canal is typically a gradual process. However, many experience pain, numbness, tingling and muscle weakness that worsens over time. Symptoms can come and go and vary from person to person.
You can experience spinal stenosis anywhere along the spinal column. However, the lower back, or lumbar stenosis, and neck, or cervical stenosis, are the most common regions, so you’re more likely to have discomfort in these areas. Other spinal stenosis indicators might include:
- Balance issues
- Loss of bladder or bowel control
- Sciatica, or pain that travels along the sciatic nerve into the lower back, buttocks or thighs
- Difficulty lifting the front part of your foot, known as foot drop
Can Spinal Stenosis Cause Neuropathy?
Yes — spinal stenosis is a potential cause of neuropathic pain. When the spaces between your spine condense, it can pinch and compress the nerves, possibly leading to neuropathy. Many people with spinal stenosis develop neuropathy secondary to this condition.
Treatment Options
Now that you know the relationship between spinal stenosis and neuropathy, you may be wondering what you can do to alleviate pain and other symptoms. Some common remedies for spinal stenosis include:
- Physical therapy or exercise: Your health care provider may suggest physical therapy sessions or exercise to build your back and stomach muscles. A physical therapist can show you gentle movements that reduce pressure on pinched or compressed nerve roots. They may also recommend range-of-motion exercises to support muscle health and stabilize the joints. This may help relieve spinal stenosis pain and make walking easier.
- Cortisone: Your doctor may inject cortisone — a pregnene steroid hormone that can help reduce pain and inflammation — into your spinal column. A cortisone injection may either bring short- or long-term relief.
- Pain relievers: Your physician may recommend over-the-counter medications like acetaminophen or ibuprofen to help manage your pain. However, more severe discomfort might call for prescription-strength medication. In some cases, doctors may even prescribe opioid medications for intense nerve-related pain. While they provide immense relief, remember that opioids aren’t intended for long-term use.
- Hot compress: Applying a heat pack to the affected region can stimulate blood flow, relieve achy joints and relax the muscles. Just be mindful of the heat setting so you don’t burn yourself and elevate the pain.
- Cold compress: Try switching to an ice pack if a hot compress isn’t easing your symptoms. Ice can reduce swelling, inflammation and tenderness. Alternate between heat and ice as needed.
When to Pursue Surgery
Most people respond well to medication and other non-surgical techniques. However, you may need spinal stenosis surgery if:
- Your symptoms persist or worsen with non-surgical treatments.
- You’re experiencing severe long-term pain, numbness and tingling in your arms or legs.
- You have a loss of sensation or reduced motor strength in your arms or legs.
- You’ve lost bladder or bowel control.
Spinal stenosis surgery helps reopen and decompress the spinal canal, which can stimulate healing and restore nerve function. You’ll likely be discharged two or three days after surgery. Your pain and inflammation should start to wear off within the first few weeks after the operation.
During recovery, your doctor will give you a list of things you can and cannot do. Try to avoid activities like lifting heavy items, housework, yardwork and high-impact exercise. Try not to sit for long durations either, as insufficient activity can also delay healing. Your physician may also recommend physical therapy.

Relieve the Symptoms of Spinal Stenosis With New York Spine Institute
If you’re experiencing spinal stenosis with neuropathy, our team at New York Spine Institute on Long Island may be able to help. We treat a variety of spine and orthopedic conditions, and we can work with you to create a personalized care plan to start your recovery.
Collaborating with your medical providers, our in-house pain management physicians and physical therapists aim to remedy spinal conditions with the most conservative methods. If surgical intervention is necessary, however, you’ll be in good hands with our world-class orthopedic spine specialists.
Whatever the symptoms or cause of your spinal stenosis, we’ll help you take your next steps in restoring your quality of life. Schedule a consultation appointment with New York Spine Institute today!
